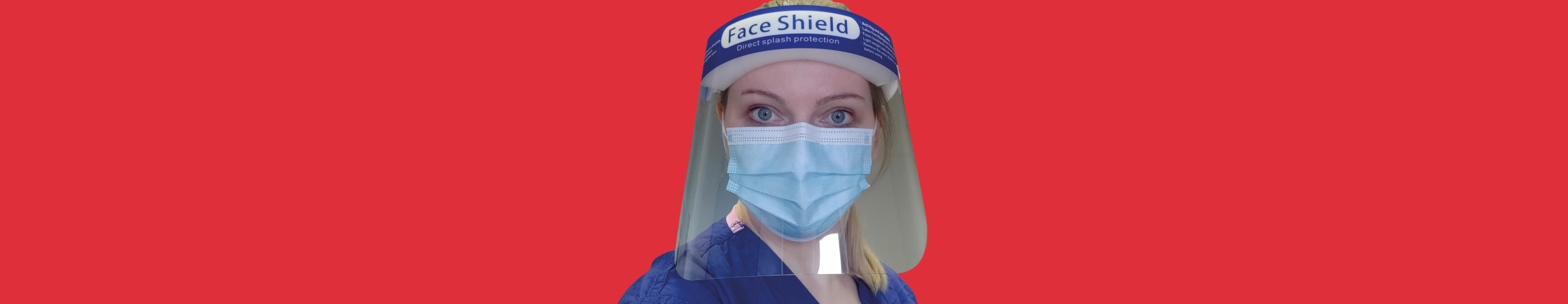
Sophie Callis (née Catt, 2009) qualified as a Clinical Psychologist three days before the first UK lockdown, and she has been working in a heart and lung hospital throughout the COVID-19 pandemic.
Last spring I was thrown in the deep end at a specialist cardiothoracic hospital, which is one of seven centres in the UK that perform lifesaving heart and lung transplants. When I started, many of the outpatient and elective services were still on hold while the hospital treated patients critically unwell with COVID-19.
Over the summer and into autumn we were able to restart much of this work, but the winter spike in infections has brought COVID-19 to the forefront of our clinical services again.
A majority of the hospital’s patients are considered ‘clinically extremely vulnerable’ and have been shielding for most of the past year. We have avoided bringing people into the hospital for appointments if it is not clinically necessary, and our hospital has made the incredibly difficult decision not to permit any visiting except under exceptional circumstances like end-of-life care. Being admitted to hospital is difficult at the best of times, but being unable to see loved ones has made it even more challenging.

We rapidly adapted to offering therapy appointments remotely via phone or video call, which has the added benefit of allowing patients living far from the hospital to access a service that they might have missed out on pre-pandemic.
For inpatients, my face-to-face work has been impacted by the personal protective equipment (PPE) that all staff are wearing throughout the hospital. None of my patients have seen my face without a mask, which means I have to work harder to show empathy and active listening – important non-verbal factors in a therapeutic relationship.
My clinical work with patients has had a huge emphasis on bringing the focus around to what they can control within a world that is so uncontrollable. My preferred therapeutic model is Acceptance and Commitment Therapy, where we accept what we cannot change and commit to acting in ways that are in-line with what is truly important to us. This lends itself well to the current global situation.
Many patients have told me how the vaccination feels like a glimmer of hope, but among the shielding population, and particularly among patients who have had transplants, there is a common theme of struggling with isolation. A donor heart or lungs can gift patients more time, but some feel that this past year has been a waste of those precious months.
Sadly, there are some patients who do not survive their illness, and it is heartrending for staff to break this news to families over the phone
Patients who have been admitted to intensive care (and particularly those who have been sedated and ventilated) often experience symptoms of anxiety, depression and post-traumatic stress even after their physical health has improved. However, surprisingly few COVID-19 patients out of those our hospital has followed-up on have needed a Clinical Psychology service. This leads me to wonder if the shared experience of COVID-19 elicits a sense of compassion that allows people to make a good psychological recovery.
Hospital employees have benefited from a strong sense of teamwork, and staff from all professions have readied themselves to be redeployed to roles where they can be most helpful.
Our hospital had a break from COVID-19 patients for a few summer months while we acted as a hub for cardiac surgery across London – but this was not a break for staff, and many NHS workers are exasperated by people ignoring lockdown restrictions and even denying the reality of the virus.
The winter spike in infections over Christmas and January has been more exhausting than the first wave. Intensive care staff are experienced in caring for patients who are critically ill, but the ICU is busier than it has ever been before. Sadly, there are some patients who do not survive their illness, and it is heartrending for staff to break this news to families over the phone and to facilitate end-of-life visits in PPE.

I have found this year incredibly challenging, but I have tried to approach this with a sense of self-compassion instead of feeling guilty. The difficulties of the last year are much bigger and longer-lasting than anything most of us have ever had to face, so we shouldn’t expect ourselves to ‘bounce back’ to normality in a short space of time.
If you have been finding lockdowns and the ongoing threat of COVID-19 difficult, please know that you are far from alone! There are some fantastic sources of support out there, and your GP can advise you on what is available locally on the NHS.
This year has made me especially proud to be part of the NHS
I’ve taken care of myself by taking breaks – lunch times, annual leave and informal chats with colleagues – and by sharing with the team, especially when there are particularly stressful days or complex patients. I have also tried to maintain a life outside of work, even though that looks very different to pre pandemic!
I’ve stayed in touch with family and friends and spent time outdoors with my husband, and I’ve kept a sense of hope for the future by having something to look forward to. I’m expecting my first child in June, which has brought a huge sense of excitement (as well as inevitable anxiety)!
Long-term I definitely want to continue working in an acute physical health setting, and I am particularly interested in intensive care psychology. Working in a clinical setting is challenging at the best of times and has exceeded anyone’s expectations during the pandemic, but this year has made me especially proud to be part of the NHS.
You can read more from Sophie in a short alumni blog from June 2020, featuring three Johnian healthcare workers.
Written by
Sophie qualified as a Clinical Psychologist in 2020 three days before the first UK lockdown. Throughout the COVID-19 pandemic she has been working in a heart and lung hospital.